Infertility affects millions of individuals and couples worldwide, cutting across age groups, geographies, and backgrounds. While it remains a deeply personal struggle, the 2026 data surrounding it reveals a broader public health reality—one that continues to evolve as medical research advances and societal patterns shift. The following statistics offer a clearer picture of the prevalence, causes, and impact of infertility today.
Infertility by the numbers: global prevalence
Infertility is far more common than many realize, touching individuals across every corner of the world.
- Infertility is a widespread global health concern, with roughly one in six people affected at some point during their lifetime—translating to an estimated lifetime prevalence of 17.5%. (WHO)

- Globally, an estimated 48.5 million couples are simultaneously affected by infertility. (NIH)
- For primary infertility—defined as never achieving a live birth—the estimated pooled lifetime and period prevalence stand at 9.6% and 9.0%, respectively. For secondary infertility—the inability to achieve an additional live birth—the corresponding figures are 6.5% and 4.9%. (WHO)
- A 2016 meta-analysis of 52 studies reported a mean global infertility prevalence of 10%, with the lowest rates recorded in Australia and the highest on the African continent. (WHO)
- Earlier estimates indicated that between 48.5 million couples globally and 186 million ever-married women in developing countries alone were affected by infertility, underscoring the scale of the issue across different population groups. (WHO)
Regional & income-level differences
Geography and economic status shape the infertility landscape in some ways, but the data also reveals surprising commonalities across borders.
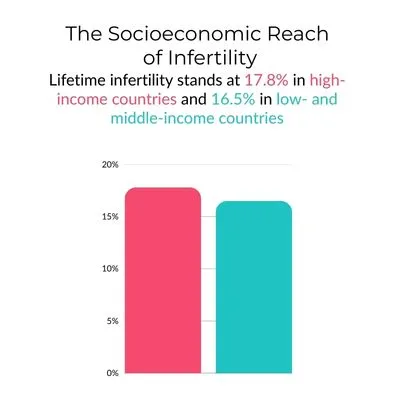
- Infertility prevalence is remarkably consistent across income levels. Lifetime infertility stands at 17.8% in high-income countries and 16.5% in low- and middle-income countries, while period prevalence is identical at 12.6% in both groups, suggesting that infertility is a universal challenge, not one confined to any particular socioeconomic context. (WHO)
- The highest estimated lifetime prevalence is found in the WHO Western Pacific Region (23.2%), while the lowest is recorded in the WHO Eastern Mediterranean Region (10.7%). In terms of period prevalence, Sub-Saharan Africa leads at 16.4%, with the Eastern Mediterranean again recording the lowest rate at 10.0%. (WHO)
- Regionally, North Africa and the Middle East—particularly Morocco and Yemen—show notably high rates of primary infertility alongside comparatively low rates of secondary infertility. In contrast, Central and Eastern Europe and Central Asia exhibit the opposite pattern, with higher secondary infertility and lower primary infertility rates. (NIH)
- While female infertility is a significant concern in developed nations, its burden is even more pronounced in developing regions, where rapid population growth and widespread industrialization contribute to environmental pressures that further threaten reproductive health. (NIH)
Female infertility: causes & contributing factors
Female infertility is rarely the result of a single cause. Rather, it stems from a complex interplay of anatomical, hormonal, genetic, and environmental factors.
Overview
Understanding the full scope of female infertility begins with its definition and its most common drivers.
- Female infertility is defined as the inability to achieve pregnancy after 12 months of unprotected intercourse in women under 35, or after just 6 months in women aged 35 or older. It remains a major global health concern, affecting nearly 15% of couples. (NIH)
- The leading cause of female infertility is fallopian tube obstruction. Secondary contributing factors include ovulatory disorders, diminished ovarian reserve, endocrine disruptions, delayed childbearing, and genetic abnormalities—with 5–10% of affected women displaying chromosomal anomalies, gene mutations, or polymorphisms. (NIH / PMC)
- In the female reproductive system, infertility may stem from a broad range of abnormalities affecting the ovaries, uterus, fallopian tubes, and the endocrine system, among others. (WHO)
Ovulatory dysfunction
Disruptions to the ovulatory cycle are among the most frequently identified causes of female infertility. PCOS alone accounts for the majority of these cases, making it a central focus of both diagnosis and treatment.
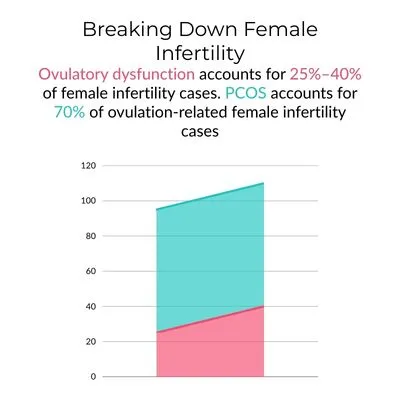
- Ovulatory dysfunction is one of the primary drivers of female infertility, accounting for 25% to 40% of cases. Polycystic ovarian syndrome (PCOS) alone is responsible for approximately 70% of anovulatory states. Additional causes include hypothalamic-pituitary disorders, hyperprolactinemia, and primary ovarian insufficiency. (NIH)
- Oligomenorrhea—irregular or infrequent menstruation—occurs in approximately 80% of women diagnosed with PCOS. (NIH)
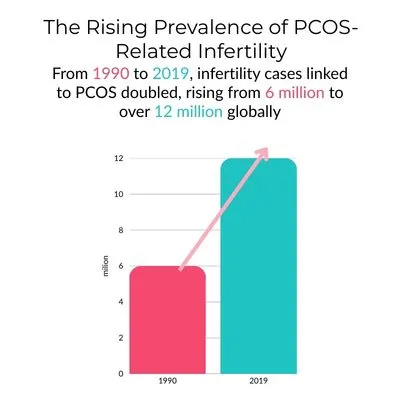
- From 1990 to 2019, infertility cases linked to PCOS among women aged 15 to 49 doubled, rising from 6 million to over 12 million globally. (NIH)
Tubal, uterine & endometriotic factors
Structural and tissue-related conditions within the reproductive system play a significant role in female infertility. These factors are often diagnosable and, in many cases, treatable.
- Tubal factors—most commonly obstruction or dysfunction resulting from pelvic inflammatory disease (PID), endometriosis, or prior pelvic surgery—are responsible for 20% to 35% of female infertility cases. (NIH)
- Uterine abnormalities, including fibroids, endometrial polyps, Asherman syndrome, and congenital malformations such as a septate uterus, account for a further 10% to 15% of cases. Endometriosis—characterized by ectopic endometrial tissue that triggers inflammation and adhesion formation—contributes an additional 10% to 15%. (NIH)
Unexplained female infertility
Even after comprehensive testing, a substantial share of female infertility cases yield no clear diagnosis. This category remains one of the most clinically challenging aspects of reproductive medicine.
- Despite thorough clinical evaluation, 15% to 30% of female infertility cases remain without a clear explanation, highlighting the diagnostic complexity of reproductive medicine. (NIH)

Male infertility: causes & health implications
Male infertility is a significant and often underestimated contributor to a couple’s struggle to conceive. Beyond reproduction, emerging research suggests it may also serve as a broader marker of overall male health.
Prevalence & causes
Male infertility is more prevalent than commonly assumed, and its causes span a wide spectrum, from identifiable and reversible conditions to complex genetic factors.
- Male factor infertility affects approximately 15% of couples worldwide and is implicated in roughly half of all infertile couples. (MDPI / AUA)
- In the United States, about 9% of men of reproductive age report experiencing fertility problems. In the United Kingdom, the estimated prevalence of male infertility stands at 10.1%. (NIH / frontiers)
- Male infertility most commonly arises from problems with semen ejection, absent or insufficient sperm production, or abnormalities in sperm morphology and motility. It contributes to 40% of infertility cases overall and is typically identified through abnormal semen analysis, defined as a sperm count below 15 million/mL or motility below 40%. (WHO / NIH)
- In approximately 30% of male infertility cases, no identifiable cause is found—a condition referred to as idiopathic male infertility. When both partners show normal evaluations yet conception does not occur, the diagnosis is termed unexplained infertility, which affects up to 25% of couples. (AUA)
- A subset of male infertility is attributable to underlying genetic conditions. The most common chromosomal cause is Klinefelter syndrome (47,XXY), which carries its own set of significant comorbidities and potential implications for life expectancy. (MDPI)
Male infertility & systemic health
The implications of male infertility extend well beyond fertility itself. A growing body of evidence links it to elevated risks of cardiovascular disease, metabolic conditions, and other serious health concerns.
- Infertile men carry a disproportionately higher burden of general health conditions. In a large Stanford study of approximately 9,387 men presenting with fertility concerns, 44% were found to have at least one significant concurrent health issue beyond their reproductive complaint. (MDPI)
- Recent meta-analytic data from 2023 indicate that men with infertility face an approximately 39% higher risk of developing type 2 diabetes and a roughly 20% greater risk of major cardiovascular events compared to their fertile counterparts. (MDPI)
- Research has also identified higher rates of chronic renal and liver disease among infertile men, along with increased rates of hospitalization and greater long-term use of prescription medications—including treatments for hypertension, diabetes, and hyperlipidemia—suggesting that infertility may be an early indicator of broader systemic health vulnerabilities. (MDPI)
- Male fertility is showing troubling declines in some populations. Among young Italian men aged 18–20, sperm counts have fallen by 25% in recent years. Currently, 33.4% of young men in this group are classified as hypofertile, while 11.7% are at risk of infertility—trends that experts link to Italy’s broader demographic challenges, where approximately 15% of couples are affected by infertility, compared to a global average of 10–12%. (unicammilus)
The role of age in fertility
Age is the single most powerful biological variable in fertility.
- The age of the female partner is the single most decisive factor in predicting a couple’s likelihood of conception. Fertility declines by nearly 50% in women in their late 30s compared to those in their 20s. (AUA)
- Women over the age of 35 are twice as likely to experience unexplained infertility compared to younger women, based on survey data involving over 7,000 participants. (NIH)
- Miscarriage risk rises sharply with age, from approximately 10% in women aged 20 to 24, to as high as 50% in those aged 40 to 44. Women between 20 and 35 also face significantly lower risks of gestational diabetes, preeclampsia, and preterm birth than those over 35. (NIH)
- Age-specific infertility data reveals a striking increase over recent decades: among women aged 35 to 39, the global prevalence of infertility rose from approximately 17 million cases in 1990 to over 30.6 million in 2021, an increase of nearly 79%. (NIH)
- From 1990 to 2021, there has been a marked global increase not only in the number of female infertility cases but also in disability-adjusted life years (DALYs), reinforcing that infertility carries a significant and growing burden on quality of life. (NIH)
- Modestly reducing body weight—by just 5% to 10%—has been shown to restore normal ovulation in 50% to 60% of obese women with PCOS, demonstrating that lifestyle interventions can have a meaningful impact on fertility outcomes. (NIH)
Conception timelines & likelihood
For most couples, conception occurs naturally within the first year of trying. Understanding typical timelines helps contextualize when medical evaluation becomes appropriate and when further investigation may be warranted.
- Most couples achieve pregnancy within the first three to six months of trying. By six months, approximately 75% of couples will have conceived. After one full year of unprotected intercourse, roughly 85% of couples will have achieved a pregnancy, a figure that rises to over 90% after two years of trying. (AUA)

- In the United States, approximately 8.8% of women of reproductive age experience infertility, while in China, over 40 million individuals are estimated to be affected, underscoring the global scale of the issue. (frontiers)
- Globally, infertility tends to be more prevalent among women than men. In the United Kingdom, the estimated prevalence is 12.5% for women and 10.1% for men. It is estimated that 20% to 30% of infertility cases can be attributed to male factors alone. (frontiers)
Assisted Reproductive Technology (ART) & treatment outcomes
Assisted reproductive technologies have transformed the possibilities for individuals and couples facing infertility.
- IVF success rates are strongly influenced by age. Women under 35 achieve live birth rates of 47% to 50% per transfer, while those over 43 see this rate drop to approximately 10%. (NIH)
- Compared to other interventions, IVF offers higher live birth rates of 40% to 50% with a lower rate of ectopic pregnancy (1.3%), while also eliminating the need for laparoscopy. (NIH)
- Advances in ART continue to improve outcomes. IVF protocols using antagonist regimens have been shown to reduce the risk of ovarian hyperstimulation syndrome (OHSS), while preimplantation genetic testing improves live birth rates by 20% in women over the age of 37. (NIH)
Psychological impact of infertility
The emotional toll of infertility is as real as its physical dimensions, yet it often goes underacknowledged. Rates of anxiety and depression among those affected are considerably higher than in the general population, and the psychological burden tends to deepen over time.
- Women experiencing infertility face a significantly elevated risk of anxiety and depression. Key contributing factors include the financial burden of treatment, advancing age, and the duration of infertility. A history of miscarriage or primary infertility further heightens the risk of depression, while limited awareness of assisted reproductive technologies is associated with increased anxiety. (NIH)
- Age is independently associated with both anxiety and depression in female infertility patients. As women age, declining oocyte quality—driven by reduced antioxidant capacity, diminished cellular energy supply, and increased apoptosis—adversely affects conception rates and raises the risk of birth abnormalities, factors that compound psychological distress. Infertile women over 35 with an urgent desire for parenthood are particularly vulnerable to depression. (NIH)
- Women with primary infertility consistently report higher levels of anxiety and depression than those with secondary infertility, indicating greater psychological sensitivity among those who have never achieved a successful pregnancy. Long-term infertility is also associated with progressive worsening of psychological symptoms over time. (NIH)
Closing remarks
Infertility is one of the most common—and most silent—health challenges of our time. Yet the data tells a story not only of prevalence and struggle, but of progress. From expanding access to assisted reproductive technologies to a deeper understanding of both male and female factors, the field continues to advance. Awareness is the first step toward change, and the numbers above make one thing clear: no one facing infertility is facing it alone.
For answers that go beyond this overview, start with the links below:
IVF Statistics Worldwide: The Figures Behind the World’s Most Hopeful Medical Journey