Miscarriage is the most common complication of pregnancy, yet it remains one of the least talked about. An estimated 23 million losses occur every year — 44 every minute — and the women behind those numbers are often left without adequate data, support, or answers. The statistics compiled here draw on the best available peer-reviewed evidence to show who is affected, when, why, and at what cost. The picture that emerges is both more common and more consequential than most people realize.
| KEY STATISTICS AT A GLANCE |
| • ~23 million miscarriages occur globally each year (44 per minute) • Pooled miscarriage risk: 15.3% of all recognized pregnancies worldwide • ~80% of all miscarriages occur before week 12 of pregnancy • Chromosomal abnormalities cause 50–67% of first-trimester losses • UK national economic cost of miscarriage: £471 million/year |
#1: An estimated 23 million miscarriages occur worldwide every year — 44 every minute
Miscarriage is not a rare event. It is the most common complication of pregnancy, yet its true scale is consistently underestimated. The 15.3% pooled global rate applies only to recognized pregnancies — when undetected early losses are included, some estimates place the real figure closer to 26%. But counting miscarriages requires systems designed to count them, and most countries do not have them.
• Around 80% of all pregnancy losses occur during the first trimester (before 12 weeks).

#2: The UK sees ~250,000 losses a year. The US has no equivalent figure
Rates vary significantly across borders, but the variation in data quality is just as striking as the variation in rates. Countries with national health registries such as the UK, Canada, Sweden can report with reasonable confidence. Countries without them, including the United States, are working from surveys and estimates. The CDC does not collect data on pregnancy losses before 20 weeks.
That absence of data has consequences: for the women who experience a loss without explanation, and for the researchers trying to understand why.
• Country-level miscarriage rates vary significantly, shaped by healthcare access, reporting standards, and population demographics.
Miscarriage rates by country
| Country | Miscarriage Rate | Notes |
|---|---|---|
| United States | 10–20% of known pregnancies | Mayo Clinic estimate; true rate likely higher due to undetected losses |
| United Kingdom | ~20% of pregnancies | ~250,000 miscarriages per year; NHS and Tommy’s data |
| Canada | 15–25% of pregnancies | Health Canada figures |
| Global average | ~15% of recognized pregnancies | The Lancet pooled analysis |
Source: J of IMAB, 2024 — International Miscarriage Rates: A Comprehensive Overview
• Countries with national health systems (e.g., UK) have significantly better miscarriage data due to standardized electronic medical records.
• In low-SDI countries, underreporting is substantial; data quality is hampered by limited infrastructure, restrictive legal environments, and inconsistent clinical definitions.
• Recurrent miscarriage rates have risen sharply in some nations. In Sweden, the number of women with recurrent losses increased by 58% between 2003 and 2012.
#3: Most miscarriages happen before many women know they are pregnant — and risk falls sharply week by week
Between 50% and 75% of all pregnancy losses occur before a positive test. By week 8, the risk for an asymptomatic woman with a normal scan has already fallen below 1.5%. Once a heartbeat is detected on ultrasound (typically around week 6 or 7), the probability of continuing past 20 weeks becomes very high for most age groups.
Timing is the single most informative number in early pregnancy. Age is the next most important, and its effect is steep.
• Roughly 80% of all miscarriages occur in the first trimester, before the 12th week of pregnancy.
• Between 50–75% of all pregnancy losses occur before a positive pregnancy test — unrecognized, and therefore absent from all clinical statistics.
• Second-trimester miscarriage rates (weeks 13–20) fall to approximately 2–3% after the first trimester ends.
• Second-trimester losses between weeks 14 and 19 range from 1% to 5% in the United States.
Miscarriage risk by gestational week
| Gestational Period | Approximate Risk | Notes |
|---|---|---|
| Weeks 3–4 (pre-positive test) | 50–75% of total losses occur here | Often undetected; attributed to heavy period |
| Week 5 | Highest pre-heartbeat risk window | Risk difficult to quantify precisely; most losses at this stage undetected |
| Week 6 | ~9.4% of women with viable scan | Risk drops sharply if heartbeat detected |
| Week 7 | ~4.2% | |
| Week 8 | ~1.5% | |
| Week 9 | ~0.5% | |
| Week 10 | ~0.7% | |
| Weeks 11–12 | ~1–2% | Risk stabilizing through end of first trimester |
| Weeks 13–20 | 1–5% (US data); ~2–3% globally | Classified as late miscarriage; structural causes more common |
| After week 20 | Classified as stillbirth | Different clinical category; different risk profile |
Source: PubMed (Tong et al., Obstetrics & Gynecology)
Source: PubMed (Wyatt et al.)
#4: Age is the strongest predictor by far: at 25-29 the risk is ~8%, and by 45 it exceeds 53%
No single variable predicts miscarriage risk more reliably than maternal age. The mechanism is largely chromosomal: as egg quality declines, the proportion of embryos with abnormal karyotypes rises steeply.
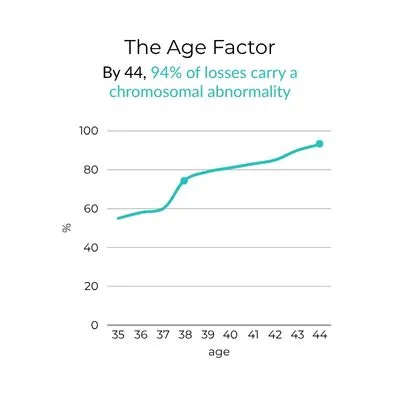
A study of 7,118 cases found that at age 38, the rate of chromosomally abnormal losses surges by nearly 15 percentage points in a single year. By 44, 94% of miscarried pregnancies in the dataset carried a chromosomal abnormality. For women who experience this more than once, the compounding weight of that statistic becomes personal.
• Maternal age is the single strongest risk factor for miscarriage, with risk rising at both extremes of reproductive life (under 20 and over 35).
• The lowest miscarriage risk is observed between ages 25 and 29, according to a Norwegian population-based study.
• Women aged 20–24 lose approximately 8.9% of pregnancies; women aged 42 lose more than half; women 45 and older face a 74.7% loss risk.
Miscarriage risk by age bracket
| Maternal Age | Miscarriage Rate | Notes |
|---|---|---|
| Under 20 (teens) | ~14% | Higher risk linked partly to socioeconomic and lifestyle factors |
| 20–24 | ~8–9% | Lowest-risk age group begins here |
| 25–29 | ~8% | Lowest risk window |
| 30–34 | ~12% | Gradual upward trend begins |
| 35–37 | ~16–20% | Risk crosses 1 in 5 threshold |
| 38–39 | ~22% | Egg quality and chromosomal errors accelerate |
| 40–41 | ~33% | Risk exceeds 1 in 3 pregnancies |
| 42–43 | ~45% | Nearly 1 in 2 pregnancies affected |
| 45 and over | 53–80% | Mayo Clinic upper estimate reaches 80% |
Source: Magnus et al. BMJ
Source: MDPI Cells, Dec 2024 — Chromosomal Abnormalities in Miscarriages and Maternal Age — 7,118 Cases
• Advanced paternal age (over 40) is also an independent risk factor for spontaneous miscarriage, confirmed by systematic review and meta-analysis.
• A study of 218,990 women (UK Biobank) found women with a history of pregnancy loss, including miscarriage, face elevated long-term risk of common mental disorders.
#5: After three consecutive losses, the risk of another reaches ~43%
Recurrent pregnancy loss (defined as two or more consecutive miscarriages) affects approximately 5% of couples trying to conceive.
The compounding emotional toll is significant: research shows that couples with recurrent loss experience more severe depression and stress for longer periods than those who have had a single loss. Despite this, nearly two-thirds of women referred to specialist centres go on to achieve a live birth within five years. Understanding why losses happen, and whether they can be prevented, is where the science becomes harder.
• Approximately 2% of women experience recurrent pregnancy loss (two or more consecutive miscarriages).
• Approximately 5% of women experience recurrent miscarriage with adverse consequences for psychological well-being and reproductive potential.

#6: Chromosomal abnormalities drive the majority of losses, but up to half of miscarriages still have no identified cause
When conventional karyotyping is used, chromosomal abnormalities are found in around 50% of first-trimester losses. When advanced genomic methods are applied to the same tissue, that figure rises to 67-68%. Autosomal trisomies — particularly of chromosomes 16, 22, and 21 — are the most common subtype.
But between 30% and 50% of miscarriages produce no identifiable cause even after full investigation, a gap that continues to drive research. What is known is that the risk factors extend beyond biology.
• Chromosomal abnormalities account for approximately 50% of first-trimester miscarriages and up to 67.25% when advanced genomic methods are applied.
• A study of 1,745 losses found 50.4% were karyotypically abnormal; when advanced genomic testing was applied, the total abnormality rate rose to 67.8%.
• Between 30% and 50% of miscarriages have no identifiable cause, even after investigation.
Chromosomal abnormality subtypes in miscarried pregnancies
| Cause | Estimated Share |
|---|---|
| Chromosomal abnormalities (total, first trimester) | ≥50% (conventional karyotyping); up to 67.8% (genomic methods) |
| Autosomal trisomies (e.g., trisomies 16, 22, 21) | 30–61% of chromosomally abnormal losses |
| Triploidy | 11–13% of chromosomally abnormal losses |
| Monosomy X | 10–15% of chromosomally abnormal losses |
| Tetraploidy | ~9% |
| Structural rearrangements | 2–6% |
| Mosaicism | ~8% |
| Uterine / structural abnormalities | ~10–15% of all miscarriages |
| Immune / clotting disorders (e.g., antiphospholipid) | ~5–10% |
| Hormonal factors (e.g., thyroid, progesterone) | ~5% |
| Unknown / unexplained | 30–50% |
Source: Fertility and Sterility (2023) — Genetic Causes of Sporadic and Recurrent Miscarriage
Source: Nature Medicine (2023) — Prevalence of Chromosomal Alterations in First-Trimester Pregnancy Loss
#7: Smoking, alcohol, night-shift work, air pollution — the confirmed risk factors extend well beyond the obvious
The Lancet series on miscarriage confirmed more than a dozen independent risk factors, several of them environmental or occupational. Iron deficiency is the only modifiable risk factor specifically flagged by the Global Burden of Disease dataset — and its impact is concentrated in low-income regions where it remains both prevalent and largely preventable. Meanwhile, the overall trend depends on where you look.
• Confirmed risk factors for miscarriage include: maternal age (under 20 or over 35), paternal age (over 40), very low or very high BMI, prior miscarriages, smoking, alcohol, stress, night-shift work, air pollution, and pesticide exposure.
Quantified risk factor data
| Risk Factor | Risk Level | Notes |
|---|---|---|
| Smoking | Elevated relative risk vs. non-smokers | Dose-dependent; associated with recurrent loss |
| Alcohol | Strongest association at <10 weeks gestation | Risk increases with quantity; type of alcohol also a factor |
| BMI — extremes | Both very low and very high BMI increase risk | Cited in Lancet as confirmed independent risk factor |
| Night-shift work | Statistically elevated risk | Mechanism likely hormonal disruption |
| Air pollution | Statistically elevated risk | Included in Lancet confirmed risk factors |
| Pesticide exposure | Statistically elevated risk | Included in Lancet confirmed risk factors |
| Paternal age >40 | Independent elevated risk | Confirmed by systematic review and meta-analysis |
| Prior miscarriage | Risk escalates with each consecutive loss | After 3 losses: ~43% risk of another (see Section 5) |
| Iron deficiency | Significant risk in low-SDI regions | Sole GBD identified modifiable risk factor |
Source: Quenby et al., The Lancet — The Lancet — Miscarriage Matters (2021)
Source: PMC (2020) — Advanced Paternal Age and Spontaneous Miscarriage — Meta-Analysis (2020)
#8: US pregnancy loss risk has been rising by 1-2% per year since 1990 — even as global rates slowly fall
The global picture and the US picture point in opposite directions. Worldwide, age-standardised miscarriage incidence has been declining — down roughly 2% annually between 2015 and 2019.
In the United States, self-reported pregnancy loss has been climbing at a similar rate throughout the same period, with metropolitan women aged 25-34 showing the steepest increase. Part of the US trend is measurement artefact: more sensitive home pregnancy tests now detect losses that went unregistered in earlier decades.
• More recent NSFG data show pregnancy loss risk continued rising by 1–2% annually, with metropolitan women aged 25–34 experiencing the fastest increase.
• Miscarriage prevalence was higher in metropolitan areas, while stillbirth was more prevalent in non-metropolitan areas.
• An earlier trend of increasing reported early losses (pre-8-week) is partly explained by the adoption of more sensitive home pregnancy tests, allowing women to identify losses previously unrecognized.
#9: 29% of women meet PTSD criteria one month after a miscarriage. At nine months, 18% still do
Miscarriage is consistently under-recognised as a psychological event. There is no routine screening for depression or PTSD after pregnancy loss in most health systems, and the social convention of not announcing pregnancy until after 12 weeks means many women grieve in silence.
The data show that clinically significant distress — at levels comparable to other major traumas — persists well beyond the immediate aftermath of the loss. That burden does not stay contained to mental health. It reaches forward into economics, careers, and future pregnancies.
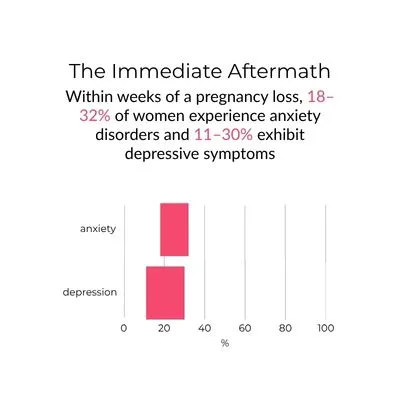
• Within 1–2 months following a pregnancy loss, 18–32% of women experience anxiety disorders and 11–30% exhibit depressive symptoms.
• 29% of women with early pregnancy loss met criteria for PTSD at 1 month post-loss; 18% still met criteria at 9 months.
• Four in ten women experienced PTSD symptoms within 3 months of either a miscarriage or ectopic pregnancy (symptoms included nightmares, flashbacks, avoidance behaviors).
• Moderate/severe anxiety was reported in 24% of women at 1 month post-loss, declining to 17% at 9 months.
• Moderate/severe depression was reported in 11% of women at 1 month, declining to 6% at 9 months post-loss.
• Women who experienced early pregnancy loss were approximately twice as likely to report moderate-to-severe anxiety and nearly 4 times as likely to report moderate-to-severe depression compared to women with viable pregnancies.
• In couples with recurrent pregnancy loss: 72.7% of women and 66.3% of their male partners showed risk of anxiety; 51% of women and 19% of male partners showed risk of depression.
• A UK Biobank study of 218,990 women followed for a median of 13.36 years found that a history of pregnancy loss — including miscarriage — was associated with elevated long-term risk of common mental disorders.
Psychological impact timeline after miscarriage
| Timepoint | Psychological Impact Rates | Notes |
|---|---|---|
| 1 month post-loss | PTSD: 29% | Anxiety: 24% | Depression: 11% | Highest acute impact window |
| 3 months post-loss | PTSD: ~39% self-reported criteria | Consistent with PTSD trajectory |
| 9 months post-loss | PTSD: 18% | Anxiety: 17% | Depression: 6% | Significant residual burden |
| Long-term | Risk elevated for years; up to 13 years documented | Mental disorders diagnosed in later life |
Source: Farren et al., Am J Obstet Gynecol (2020) — Posttraumatic stress, anxiety and depression following miscarriage and ectopic pregnancy — multicenter prospective cohort study
#10: The UK’s annual miscarriage bill exceeds £471 million. The US equivalent is unknown, because the data does not exist
The £471 million figure for the UK covers short-term healthcare costs only — emergency visits, surgical procedures, follow-up care. It does not capture lost earnings, reduced career progression, or the long-term healthcare burden from increased risk of preterm birth, cardiovascular disease, and mental health treatment in subsequent years.
In the United States, no equivalent national figure exists, because the CDC does not collect or publish data on pregnancy losses before 20 weeks. The losses continue past the pregnancy itself — into the body, and into future ones.
• The short-term national economic cost of miscarriage is estimated at £471 million per year in the UK.
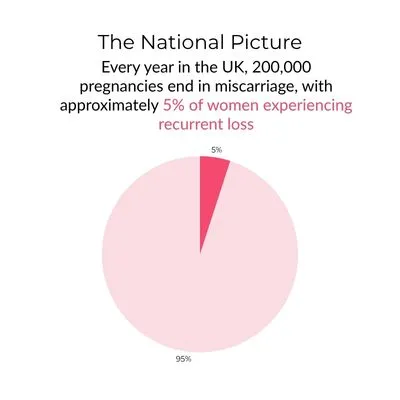
• There are approximately 200,000 miscarriages per year in the UK, with approximately 5% of women experiencing recurrent loss.
• US women who experienced a first miscarriage worked approximately 200 fewer hours per year afterward, translating to an annual income reduction of approximately $5,000 per year over 7 years post-loss.
• Declining mental health following miscarriage may lead to short-term lower probability of career promotion and salary stagnation.
• Comprehensive US cost data is not available because the CDC does not publish miscarriage statistics for losses before 20 weeks gestation.
#11: A history of miscarriage raises the risk of preterm birth, placental complications, and cardiovascular disease — not just another loss
Miscarriage does not end when the pregnancy ends.
Research has established it as a sentinel risk marker for a range of future obstetric complications and, in cases of recurrent loss, for long-term conditions including cardiovascular disease and venous thromboembolism. Women with three or more prior losses face the highest risk of preterm birth in any subsequent pregnancy.
Yet nearly two-thirds of women with recurrent loss who receive specialist care will achieve a live birth within five years. What remains is the question of how well any system is designed to support them while they try.
• Miscarriage and especially recurrent miscarriage is a sentinel risk marker for preterm birth, fetal growth restriction, placental abruption, and stillbirth in future pregnancies.
• A history of recurrent miscarriage is also a predictor of longer-term health problems including cardiovascular disease and venous thromboembolism.
• The risk of preterm birth increases with each previous miscarriage; women with three or more prior miscarriages are at the highest risk.
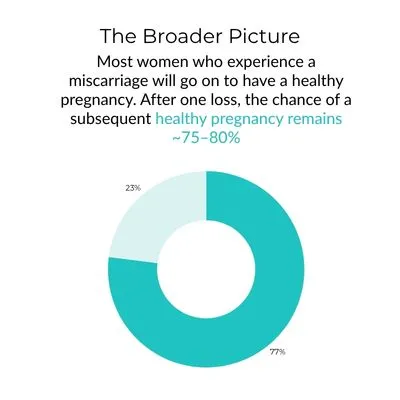
• Most women go on to have successful pregnancies after a single miscarriage. After one loss, the chance of a subsequent healthy pregnancy remains approximately 75–80%.
• Almost two-thirds of women with recurrent miscarriage referred to a tertiary centre succeeded in having at least one live birth within 5 years of first consultation.
• Pooled prevalence of fetal chromosomal anomalies in women with recurrent pregnancy loss (39%) was comparable to that found in sporadic miscarriages (45%) — suggesting similar underlying genomic mechanisms.
• Women with PTSD following miscarriage are at higher risk of prenatal loss, pregnancy complications, ectopic pregnancy, preterm birth, and growth abnormalities in subsequent pregnancies.
#12: Missing data, missing answers: the global surveillance gap in pregnancy loss
Countries with national health systems (like the UK, Norway, Sweden) have been able to conduct large-scale, longitudinal studies on miscarriage precisely because they have standardised registries.
• The CDC does not publish federal miscarriage statistics for pregnancy losses occurring before 20 weeks gestation, creating substantial national data gaps.
• Self-reported pregnancy loss rates in the US (NSFG data) show a 19.7% loss rate, considerably higher than the 10–20% clinically recognized figure illustrating the divergence between self-report and clinical surveillance.
• In low-SDI countries, underreporting of miscarriage incidence and mortality is driven by restricted healthcare access, inconsistent legal definitions, and under-resourced surveillance infrastructure.
• Increasing use of more sensitive home pregnancy tests means that some apparent ‘increases’ in early miscarriage rates are likely an artifact of better detection, not a true biological increase.
• Temporal changes in clinical definitions, diagnostic practices, and reporting systems have influenced long-term trend comparisons across countries and time periods.
What the numbers tell us
Somewhere in the figure of 23 million annual losses is a woman who did not know she was pregnant. Another who had three losses before this one. Another who will spend the next nine months meeting the clinical criteria for PTSD, with no routine follow-up offered and no system in place to notice.
The statistics above describe a condition that is common, consequential, and still poorly served by the institutions that should be tracking it. Risk is fairly predictable, influenced by age, chromosomal abnormalities, and timing, with the most reassuring sign being the confirmation of a heartbeat. And yet, for up to half of all cases, no cause is ever found.
What most women want to know after a miscarriage is why it happened and whether it will happen again. For a significant proportion of them, the data we have does not yet provide an answer.
Closing that gap in research, in reporting, and in the care that follows is where the real work remains.
What the infertility data actually shows
Infertility Statistics 2026: The Data Behind a Widespread Health Issue
IVF Statistics Worldwide: The Figures Behind the World’s Most Hopeful Medical Journey
Primary sources used in this article
- https://pubmed.ncbi.nlm.nih.gov/33915094/
- https://pubmed.ncbi.nlm.nih.gov/40287625/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC5771868/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC12477614/
- https://www.nature.com/articles/s41591-023-02645-5
- https://pubmed.ncbi.nlm.nih.gov/39791709/
- https://www.sciencedirect.com/science/article/pii/S001502822301720X
- https://pubmed.ncbi.nlm.nih.gov/31953115/
- https://www.frontiersin.org/journals/psychiatry/articles/10.3389/fpsyt.2024.1326894/full
- https://pmc.ncbi.nlm.nih.gov/articles/PMC9937061/
- https://www.journal-imab-bg.org/issues-2024/issue3/vol30issue3p5703-5709.html
- https://www.statnews.com/2024/08/21/miscarriages-poor-data-researchers-explore-causes/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC4610348/
- https://pubmed.ncbi.nlm.nih.gov/18310375/
- https://www.phc.ox.ac.uk/research/groups-and-centres/health-economics-research/economic-costs-associated-with-miscarriage-a-secondary-analysis-of-qresearch
- https://pubmed.ncbi.nlm.nih.gov/30422585/
- https://pubmed.ncbi.nlm.nih.gov/22183209/
- https://pubmed.ncbi.nlm.nih.gov/30894356/
- https://www.mayoclinic.org/diseases-conditions/pregnancy-loss-miscarriage/symptoms-causes/syc-20354298
- https://www.marchofdimes.org/find-support/topics/miscarriage-loss-grief/miscarriage
- https://en.wikipedia.org/wiki/Miscarriage_and_mental_disorders